How to Tell If Your Pain Is Arthritis or Not
Joint pain is incredibly common but not all joint pain means arthritis.
In fact, millions of people worry they have rheumatoid arthritis or osteoarthritis, when the cause might be something completely different. Understanding the difference can feel overwhelming, especially when your hands, knees, or feet start hurting and you don’t know what your body is trying to tell you.
As a rheumatologist, one of the most common things I hear from patients is:
“Doctor, I think I just have arthritis… right?”
Sometimes yes.
Sometimes no.
And knowing the difference early can protect your joints, prevent damage, and guide you to the right treatment faster.
Let’s walk through this together, clearly and calmly.
Is It Arthritis or Just Joint Pain?
Before jumping to conclusions, here’s the key truth:
Joint pain is a symptom. Arthritis is a diagnosis.
Not every ache equals arthritis.
Pain can come from:
Tendons
Ligaments
Muscles
Bursae
Or the joint itself
So the first step is understanding where the pain is coming from.
What Exactly Is a Joint? (And Why It Matters)
Think of a joint like a well-oiled hinge.
It includes:
Two bones
Cartilage (cushion)
Synovial fluid (lubrication)
Synovial lining (joint lining)
Ligaments and tendons for support
When everything is healthy → movement is smooth and quiet.
When something goes wrong → pain, stiffness, swelling.
Different types of arthritis affect different parts of the joint. That’s why symptoms feel different between rheumatoid arthritis and osteoarthritis.
Causes of Joint Pain That Are NOT Arthritis
Before we even talk about arthritis, remember:
Many common pains aren’t arthritis at all.
Examples:
Rotator cuff tendonitis (shoulder)
Bursitis
Muscle strain
Tendon injuries
Overuse
These often improve with:
Rest
Physical therapy
Ice/heat
Strengthening exercises
If pain resolves quickly, it’s usually not arthritis.
Rheumatoid Arthritis vs Osteoarthritis: What’s the Difference?
This is where most confusion happens.
Both cause joint pain.
But they behave very differently.
Let’s break it down simply.
Osteoarthritis (Wear-and-Tear Arthritis)
What is it?
Osteoarthritis happens when cartilage slowly wears down over time.
Think: “mileage” on your joints.
Common areas
Knees
Hips
Lower back
Hands (finger joints)
Feet
Typical symptoms
Pain worse with activity
Better with rest
Morning stiffness < 30 minutes
Bony enlargement
Minimal warmth
Gradual progression
Real-life example
You walk all day → knees ache at night → feel better the next morning.
That’s classic osteoarthritis.
Quick Clues It Might Be Osteoarthritis
✅ Pain increases with use
✅ Stiffness short-lived in morning
✅ Localized swelling
✅ No fatigue or whole-body symptoms
✅ Age-related or prior injury
Rheumatoid Arthritis (Inflammatory Arthritis)
What is it?
Rheumatoid arthritis is an autoimmune disease.
Your immune system mistakenly attacks the joint lining (synovium).
This leads to:
Inflammation
Swelling
Joint damage
Deformities if untreated
Common areas
Hands
Wrists
Feet
Small joints
Often symmetrical
Typical symptoms
Morning stiffness > 30–60 minutes
Soft swelling
Warm joints
Fatigue
Low energy
Pain improves with movement
Real-life example
You wake up feeling stiff like you “can’t open your hands,” but once you move around, you feel better.
That’s classic rheumatoid arthritis.
Quick Clues It Might Be Rheumatoid Arthritis
✅ Long morning stiffness
✅ Swollen, warm joints
✅ Pain improves with activity
✅ Fatigue
✅ Multiple joints involved
✅ Symptoms on both sides of the body
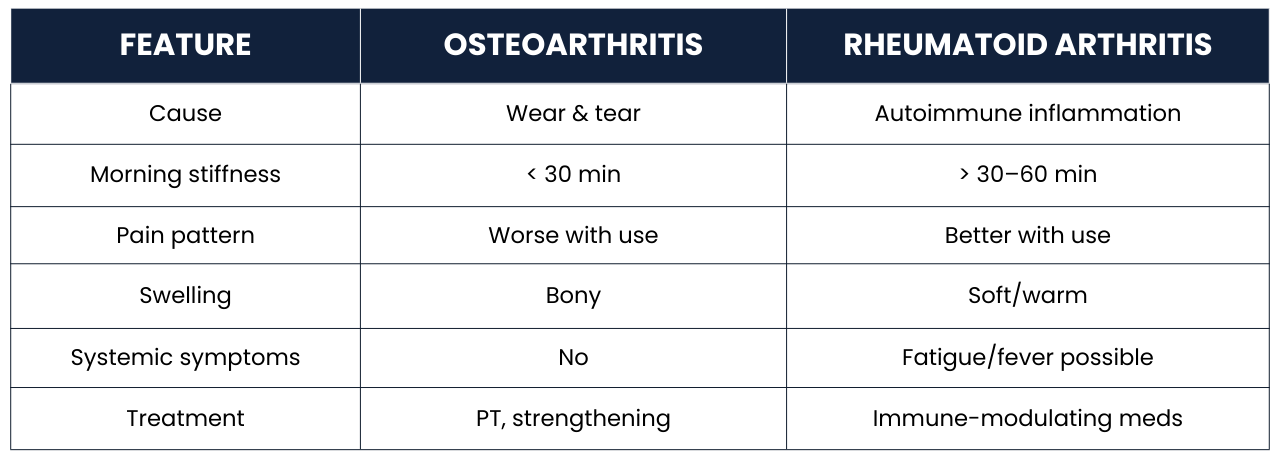
Side-by-Side Comparison: Rheumatoid Arthritis vs Osteoarthritis
When Should You See a Doctor for Joint Pain?
Don’t ignore persistent symptoms.
Seek medical care if:
Pain lasts > 6 weeks
Joints swell repeatedly
Morning stiffness lasts > 30 minutes
Both hands/feet hurt
You feel fatigued or “flu-like”
Function is declining
Early diagnosis is especially critical for rheumatoid arthritis, because untreated inflammation can permanently damage joints.
And once damage happens, we can’t reverse it.
Why the Right Diagnosis Matters
Here’s the big picture:
Osteoarthritis → movement helps
Rheumatoid arthritis → medication is essential
Treating inflammatory arthritis like “wear and tear” delays proper care.
That delay can mean:
Joint deformity
Loss of mobility
Chronic pain
Early treatment = better outcomes.
Always.
Practical Tips Before Your Appointment
Bring this info to your doctor:
When did pain start?
How long is morning stiffness?
Which joints hurt?
Better with rest or movement?
Any fatigue or fever?
This helps your doctor quickly determine if it’s rheumatoid arthritis, osteoarthritis, or something else entirely.
FREQUENTLY ASKED QUESTIONS
-
Yes. Tendonitis, bursitis, and muscle strain commonly cause joint-area pain without arthritis.
-
Usually more than 30–60 minutes.
-
No. Osteoarthritis frequently affects the hands too.
-
Yes, but it’s typically bony, not warm or inflamed.
-
If pain persists, joints swell, or stiffness lasts over 30 minutes in the morning.
Listen to Your Joints
Joint pain is your body’s alarm system.
It’s how your body says, “Something isn’t right.”
Sometimes it’s simple wear-and-tear osteoarthritis that improves with movement, strength training, and joint protection.
But sometimes it’s rheumatoid arthritis — an inflammatory autoimmune disease that needs early medical treatment to prevent permanent joint damage.
And here’s the truth most people don’t hear soon enough:
Waiting too long can make arthritis harder to treat.
Joint damage from rheumatoid arthritis can be irreversible.
The earlier you get evaluated, the better your outcomes.
So if you’re experiencing:
Persistent joint pain
Hand pain or wrist swelling
Morning stiffness longer than 30–60 minutes
Warm or puffy joints
Fatigue with joint symptoms
Pain affecting both sides of your body
Please don’t guess or self-diagnose.
Talk to a Rheumatologist
Getting the right diagnosis early means:
Less pain
Less joint damage
Better mobility
Better quality of life
If you’re looking for a rheumatologist near Cary, NC and want clear answers about your joint pain, rheumatoid arthritis, or osteoarthritis symptoms, you can book an appointment through www.empoweredarthritis.com for a comprehensive evaluation and a personalized care plan tailored to you.
If you’re outside North Carolina or the United States but still want guidance, you can schedule a one-on-one coaching session with me. I’d be happy to answer your questions, provide clarity, and help you create a plan so you can feel more confident about your next steps.
If you prefer to learn first, I’ve created free resources for you:
📘 Grab a copy of The Holistic Rheumatoid Arthritis Guide for step-by-step support
🥤 Download my FREE Rheumatoid arthritis pain relief smoothie recipe
My goal is simple:
To move you from pain → clarity → confidence → control.
You don’t have to live confused about your symptoms.
You deserve answers.
You deserve relief.
And you deserve a plan.
Schedule your appointment or explore all the resources today, your joints will thank you.